Almanac's Mary Lahammer Gets an Antibody Test for COVID-19
She also talks to a physician about the differences in tests and who should ultimately be tested for antibodies.
Story published: May 11, 2020
The day begins on a beautiful spring morning - it’s hard not to feel optimistic when you have trees blooming and birds chirping all around. I'm getting ready to head down to the Mayo Clinic to get the COVID-19 antibody test.

The drive down to Rochester, Minn., is a journey I’ve done many times as an MS (multiple sclerosis) patient, but, in fact, my health is so good that I haven’t had to make the trip very often. I usually bring a family member - I like to have the company and someone else to help digest the information I receive. But this time, I decided to go it alone. I didn’t want to risk any exposure to family members who usually accompany me. So here goes.
Editor’s Note: As the COVID-19 crisis unfolds in Minnesota, certain details in our stories about the impact of the virus may become outdated within hours, days or weeks of our publication. For the most up-to-date information about the coronavirus in Minnesota, please visit the websites for the Office of Governor Tim Walz and Lt. Governor Peggy Flanagan or the Minnesota Department of Health.
First, let's talk about the science with Dr. Bharat Thyagarajan from the University of Minnesota Medical School. There have been good and bad tests flooding the market - not all of the immunity tests are created equal. The doctor is skeptical about the rapid tests, though he does trust the tests that came out later, have FDA approval and take longer to run because they have better sensitivity for COVID-19 without as much cross-reacting. He says that the tests underway at Mayo and U of M have undergone fairly extensive validation.
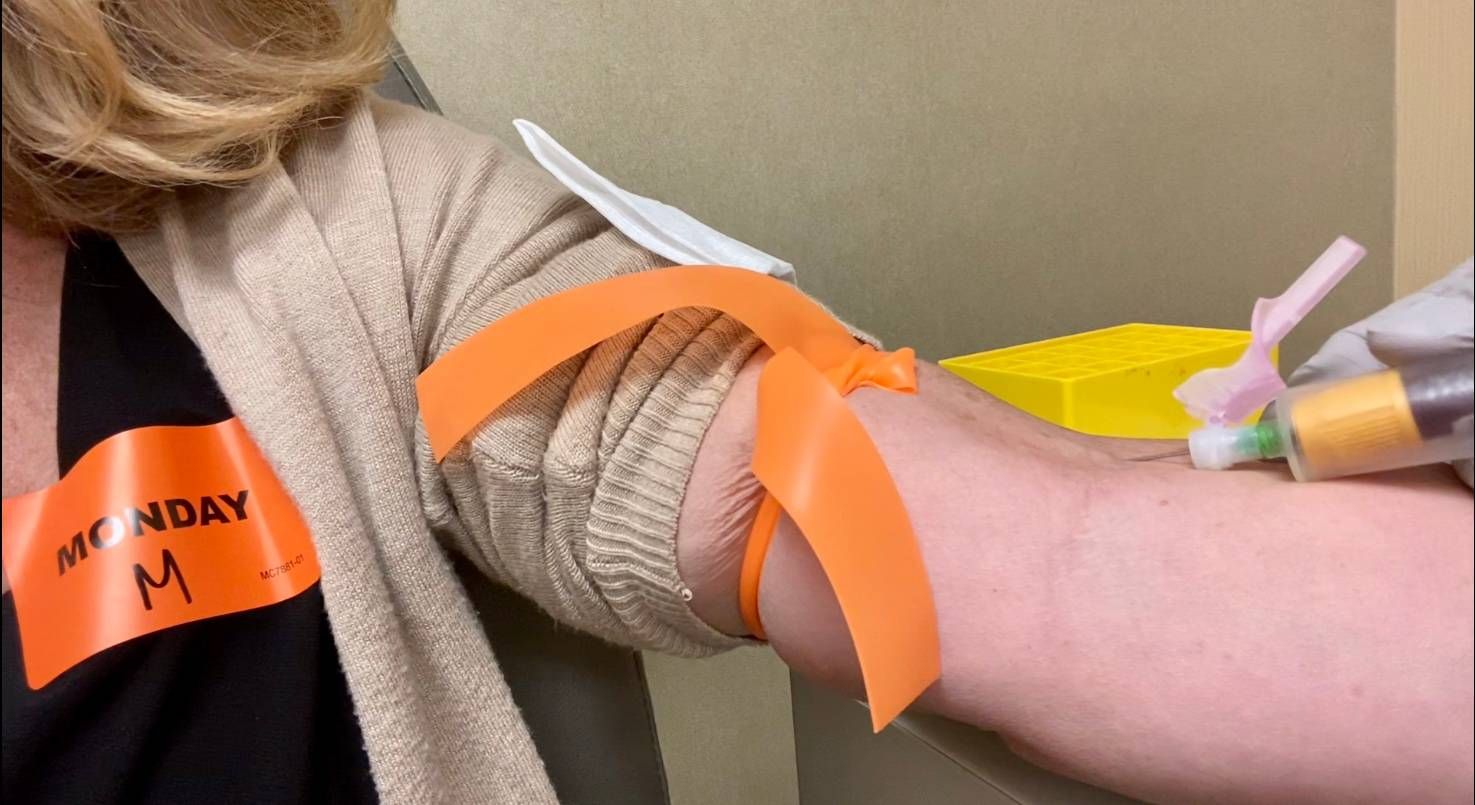
At the blood donation building on the extensive Mayo Clinic campus, my blood draw is straight-forward and doesn't take long at all. Now we wait for results.
What is less promising of late is the confidence in the staying power of antibodies or immunity. Dr. Thyagarajan doesn’t know the answer to that question and acknowledges that, "All we can say at this point is you’ve had exposure to COVID in the past. What it means for the future is really unclear. We hope antibodies will provide some level of immunity, but the data on this is not yet available." At this point in the flurry of global research, experts hold out the most hope in plasma donations from people who carry the antibodies as one way to help people with active cases.

So why I’m having this antibody test? Back in February, I contracted a severe upper respiratory illness, and then my husband quickly got it afterwards. He noted that, for weeks, he lost his sense of taste, an unusual experience to say the least. When I shared my symptoms and circumstances with my doctor here at Mayo, he ordered the immunity test for me. My aim is to know whether or not I’m at all immune - for my colleagues, for the public I interact with in my work at the Capitol - and to maybe be able to donate my plasma if I can help save lives. We hope to get results within about a day.
Dr. Thyagarajan thinks that people working in essential professions should get this test. "Yes, I think it does definitely make sense. When I said high-risk people - I tend to think of them as healthcare workers, but they are not the only people who are at high risk. First responders, cops, people working in grocery stores, journalists."
His advice for the general public, people who may be watching and want to get the antibody test themselves? "If you want to get the antibody test, do that in consultation with your physician and not outside of the healthcare system."
About a week later, test results are in, and I find out I'm negative for the antibodies. My doctor says especially since my flu test was negative, it's possible I had A coronavirus, but not THE COVID-19 coronavirus.
Diagnosing and treating patients with the novel coronavirus comes with different challenges for rural and regional healthcare systems located outside major metropolitan areas. One Greater Minnesota reporter Kaomi Goetz interviewed Essentia Health’s Chief Medical Officer Dr. Peter Henry to find out more about how rural healthcare providers are getting ready for an influx of coronavirus cases.
As the approximately 6 million pregnant women in the U.S. face uncertainty due to COVID-19, one Twin Cities PBS producer plans to chronicle her story and that of others along the way. Check out Pregnancy in the Time of Coronavirus.
As part of her reporting on the impact of the coronavirus in Minnesota, Mary Lahammer spoke with Commissioner of IT Services Tarek Tomes on the ways in which the pandemic has put a spotlight on the state's already challenging inequities. One issue that laced through their conversation? Minnesota's growing digital divide.
